Did you know that Tuberculosis (TB) is preventable and curable, but still a major problem in India? This blog explains important facts about TB, and describes how DEVI works to reduce the burden of TB in poor communities in Lucknow.
About TB
The WHO reports that in India during 2021 there were 30 lakh new cases of TB, and 5 lakh deaths from TB.
View more: data from WHO about TB in India
Many TB patients are too sick to study, do household tasks, or earn money. TB is a burden on the whole family, through added expenses, loss of income, and time taken for treatment and recovery.
How TB spreads
TB is an airborne bacterial disease – it is caused by a bacteria which enters the body through breathing infected air. Being infected with TB does not immediately cause sickness. In India about 40% of the population (50 crore people) carry the TB infection but are not sick – this is latent TB.
Latent TB can become TB disease (active TB) any time. Active TB most commonly affects the lungs (pulmonary TB) but can appear almost anywhere in the body.
TB is spread by people with active pulmonary TB, as they breathe and cough the TB bacteria into the air.
TB does not spread by
- touching the patient or their things
- eating with the patient
- patients with extra-pulmonary TB (not in the lungs)
- patients who have already taken anti-TB medicines for at least 3 weeks
Risk Factors
 Anyone of any age, religion, caste and class can get TB.
Anyone of any age, religion, caste and class can get TB.
However, these factors greatly increase the risk of TB:
- being undernourished (see INFO BOX below)
- over-crowded accommodation
- alcohol, drug and tobacco addiction/ abuse
- HIV/AIDS, diabetes (sicknesses that reduce immunity)
- cancer treatment that reduces immunity
In India, being undernourished is the biggest risk factor for TB disease, and it also reduces the success rate of treatment. Therefore ending TB in India requires nutritional support for TB patients, and addressing under-nutrition so that fewer people get TB.
INFO BOX
Undernutrition can be measured in different ways. The easiest is to calculate BMI (Body Mass Index), which compares weight to height. For pregnant women, or people with major swelling, MUAC (mid-upper arm circumference) is used. Measuring iron is also helpful, because many TB patients are anaemic, which reduces the success of treatment.
| Measure | How to calculate | Normal | Undernutrition | Extreme |
|---|---|---|---|---|
| BMI | weight (kg)/height (m) squared | 18.5-25 | 14-18.5 | <14 |
| MUAC | measure around the arm midway from shoulder to elbow | >23 cm | 19-23 cm | <19cm |
| Iron | Blood test for Haemoglobin | <13 g/dl | 7-13 g/dl | <7 g/dl |
 Symptoms
Symptoms
The most common symptoms of any type of TB are:
- loss of appetite and unexpected weight loss
- fever, especially in the evening
- night sweating
- fatigue and weakness
| Pulmonary TB | Extrapulmonary TB |
|---|---|
For pulmonary (lung) TB other symptoms are:
|
TB in other parts of the body may cause pain, swelling or other problems in that part, eg headaches, bone pain, swelling on the neck, abdominal pain. |
Diagnosis & Treatment
The most common tests for TB are chest x-rays and sputum tests (free at most government hospitals). Other tests are needed for extra-pulmonary TB. Sometimes diagnosis is done on the basis of symptoms only, without other tests.
It is very important for a TB patient to receive correct and complete treatment. The medicines are free from DOTS centres (in hospitals, clinics, public health centres, etc) and must be taken every day for 6 months, or sometimes longer. Within a few weeks of starting treatment, the patient will begin to feel much better, and TB is no longer contagious.
The government of India also provides a financial supplement of Rs500 per month, to help patients have adequate nutrition during treatment.
If TB is not properly treated, there is greater risk of death, spreading the disease to others, and developing drug-resistant TB.
TB Targets
The WHO has set targets and made a plan to eradicate TB globally by 2030. The Indian government has committed to ending TB by 2025, but COVID-19 has been a major set-back. We are not on target to reach these goals, and a lot more needs to be done …
Action on TB
To end TB in India, we need to break the cycle of TB infection in three ways, as illustrated in the diagram below.
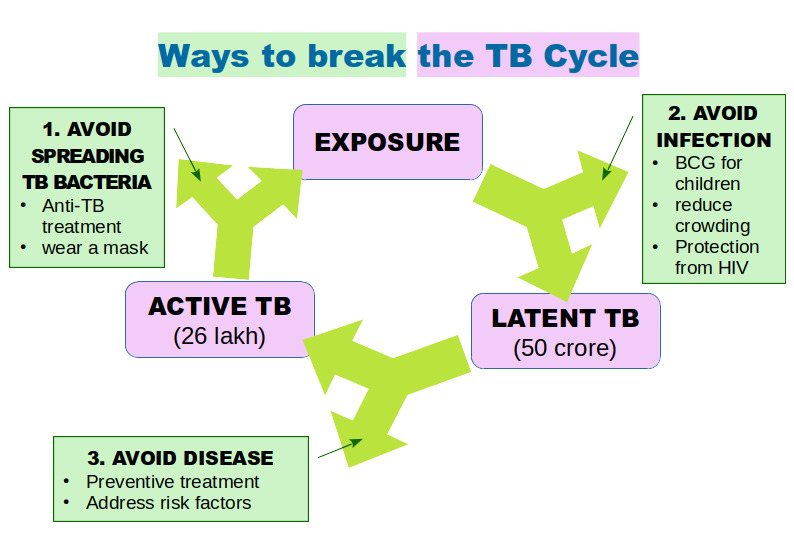
Even if every Indian with active TB completes anti-TB treatment, new cases will still occur because so many people are already infected. To end TB we must also address the risk factors, so that fewer people with latent TB will develop active TB.
What DEVI does
DEVI does not provide medical services, but works to reduce the burden of TB on poor people through the following activities:
Community Education
- awareness sessions about TB for schools, community groups, neighbourhood associations, etc
- community events for World TB Day, and to celebrate TB patients completing their treatment
- door-to-door survey of poor neighbourhoods, to educate residents and refer them for diagnosis if they have symptoms of TB
Patient Support
- visiting families of TB patients to share information and help them face challenges
- accompany patients to medical appointments
- help the patient with documents such as aadhaar card, bank account, and ration card
Addressing Risk Factors
- The community development work of DEVI takes steps to address the major risk factors for developing active TB:
- helping people access free and low cost medical services, so that diabetes, HIV, cancer and other illnesses are detected and treated as soon as possible
- referring people to de-addiction services, and encouraging less consumption of alcohol, tobacco and other drugs
- facilitating access to ration cards, pensions, and other government schemes that help provide income security and food security, to reduce under-nutrition
What YOU can do
To end TB, society wide action is needed. You can take action to help reduce the burden of TB on the nation, through local action in your own city or neighbourhood.
Community Awareness
After reading this blog, you already know more about TB than most people! Please pass on correct information to help dispel old myths about TB and how it spreads.
Action point: download this simple brochure in Hindi to print and distribute.
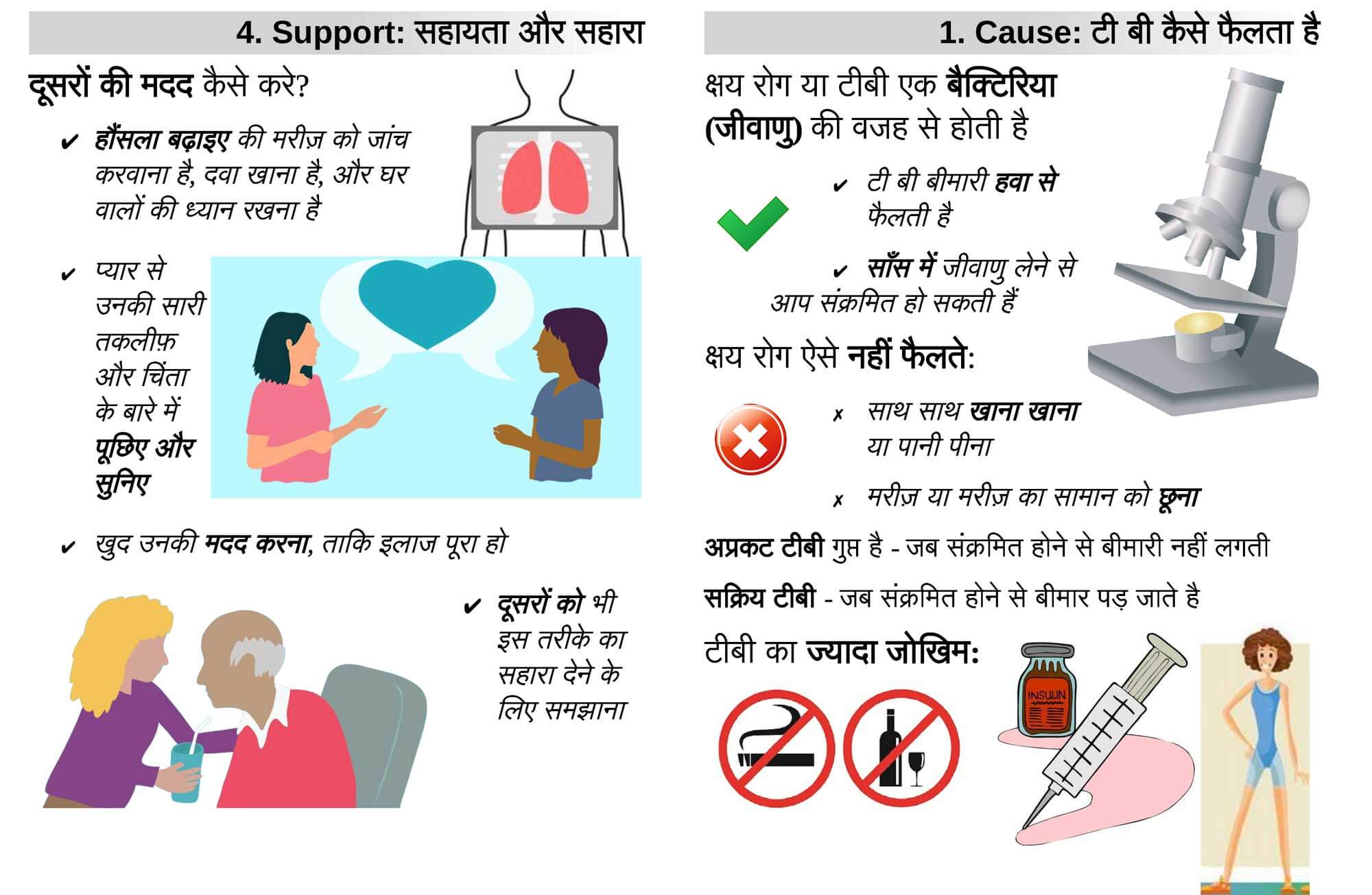
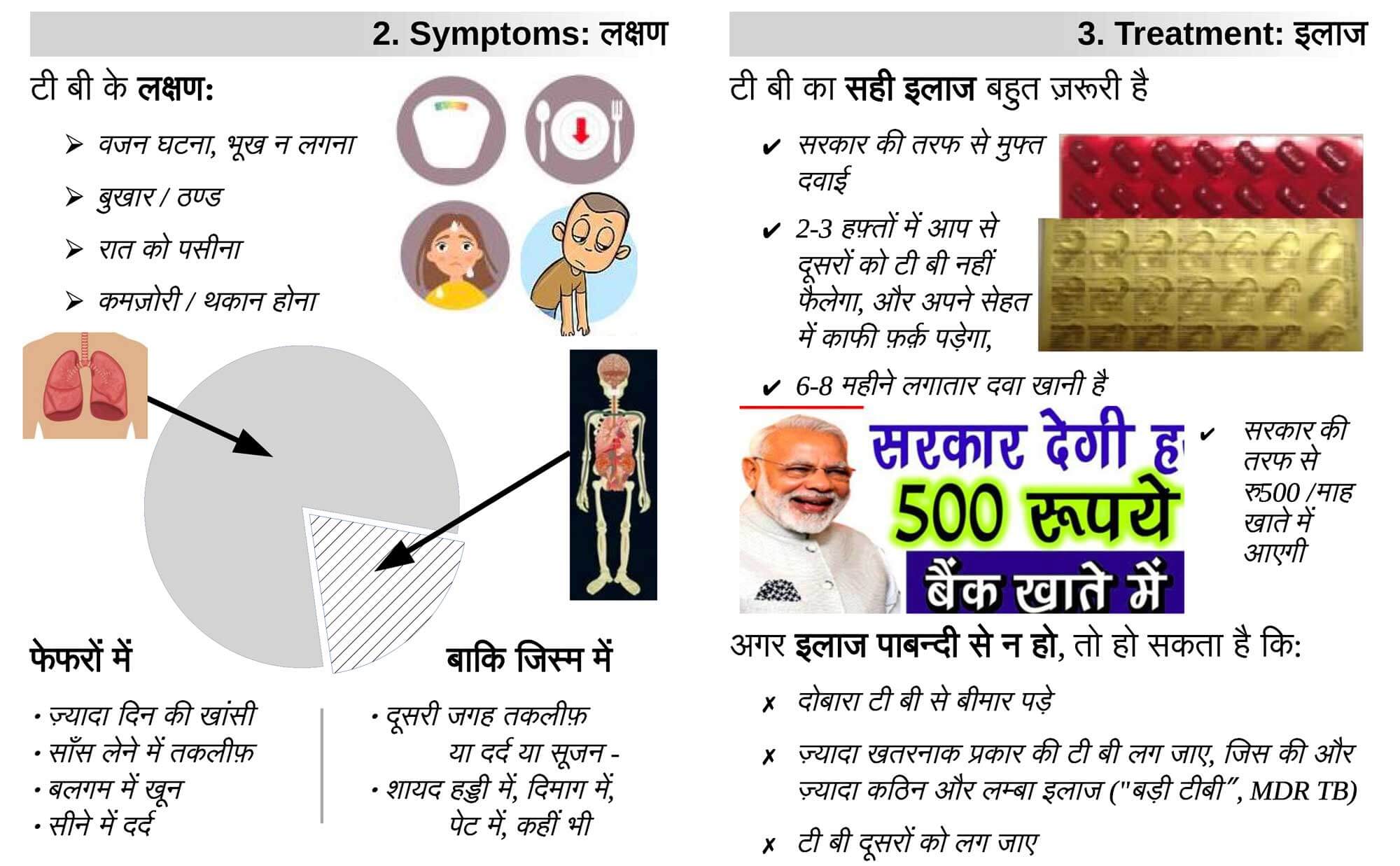
Supporting Patients
If a friend or family member has TB, you can support them to recovery – the above brochure outlines basic information and simple points about supporting patients.
Maybe you can use your professional skills or business to support TB patients with their needs:
- counsellor: hearing problems and guiding patients and their household members
- grocer shop owner: provision of monthly rations pack for patients
- medical store owner: provision of symptomatic relief medicines, multi-vitamins etc in addition to the free government anti-TB treatment
- bank branch manager: opening bank accounts and solving any account problems for TB patients
- Jan Sewa Kendra: helping TB patients to ensure they have aadhaar card, ration card and bank account, with correct current details, so they can avail the relevant government assistance
Action Point: if you don’t know anyone with TB, you can register as a Nikshay Mitra to support TB patients.
Supporting our Work
You can support our work by volunteering or donating.
Please join us in the struggle to end TB!

Nice pic of many more returns
thanks a lot